Understanding the difference
Total knee replacement which is also known as the knee arthroplasty is a common orthopaedic procedure that is used to replace the damaged joint with an artificial one. The purpose of replacement is to relieve pain and increase mobility.
Partial knee replacement surgery, on the other hand, uses a smaller incision and has a faster recovery than full knee replacement surgery. It is minimally invasive surgery that aims to remove only the most damaged areas of cartilage from the joint leaving the other healthy parts of the joint as it is. In a total knee replacement, all of the cartilage is removed from the knee joint, and an artificial or man-made metal and a plastic implant is inserted.
Benefits
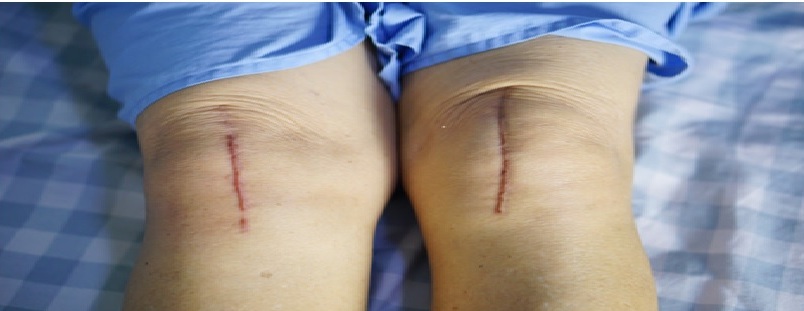
There are multiple benefits of selecting a partial knee replacement surgery over a total knee replacement surgery. While a total knee replacement surgery involves an incision of 8 inches, partial knee replacement surgery involves a minimal invasion of 4 inches only. This helps in less blood loss and quicker recovery. Patients post partial knee replacement surgeries are known to have been discharged on the day of the procedure, although most often patients are discharged on the first or second postoperative day. With traditional total knee replacement, patients are not allowed to leave before three days from the hospital, till the time the doctor gives a go ahead.
The movement of the knee joint is dependent on the interaction of the joint surface, ligaments, muscles, and tendons that surround the joint. When a total knee replacement is performed, many of these structures are removed to allow for insertion of the artificial knee joint. In a partial knee replacement, more of these structures remain, and the mechanics and movement of the joint remain more normal. Studies have clearly demonstrated that in people who have had a full knee replacement on one side and a partial on the other side, their partial knee replacement feels more “normal.”
Other than this, a minimally invasive partial knee replacement is designed for patients who have a problem of severe arthritis of the knee and who have not found relief with the standard non-surgical alternative treatments. These treatments may include physical exercises, medicines (steroids and non-steroids) and weight loss procedures.
After a partial knee replacement surgery, a patient may take anywhere between four to six weeks of physical therapy to get back to their normal routine, however, after a total knee replacement surgery, a patient may take four to six months to recover.
In terms of cost, both the surgeries are expensive, but partial knee replacement costs anything between INR 1,50,000 To 2,20,000 as compared to a total knee replacement which costs around INR 2,00,000 To 3,80,000.
Risks
Unlike traditional total knee replacement surgery, the minimally invasive partial knee replacement technique is not suitable for all patients. The patients ideal to undertake a partial knee surgery belong to the age group above 55 years but a minimal level of deformity.
Some patients suffering from arthritis also take a lot of time deciding whether to go for surgery or not. This further degrades their condition, making them reach an advanced stage which may not be treated with partial knee surgery. If partial knee replacement is done in a patient who has crossed the minimal level of arthritis, failure rates can be high, and a total knee replacement surgery will be necessary in this case.
Other factors which can actually decide whether one should opt for a total knee surgery instead of partial depends on their weight, non-aligned knee or ruptured knee ligament. This will, however, be suggested by a doctor only. There is often a temptation to have a partial knee replacement because it is less invasive and the recovery is faster. However, it is important not to overlook the long term results; a fast recovery is of no benefit if it doesn’t make one better or doesn’t last for a longer period of time. After all, every surgery involves a person’s time, cost and effort.
In case of an unsuccessful surgery or further complications like infection, blood-clotting, swelling, stiffness may occur post partial knee surgery. This may lead to another unavoidable partial surgery or total knee surgery.
Thus, partial knee surgery is not recommended for all. Your doctor is the best person to advise you on the best possible surgery as per your particular body need or medical condition. Please follow their instructions to stay active and healthy.